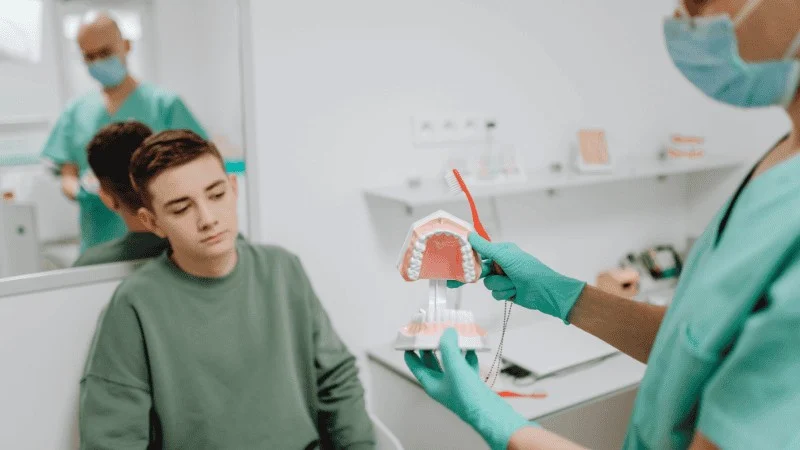
You want dental implants, but you have heard that bone loss can cause problems. After you lose a tooth, your jawbone can shrink over time. If the bone becomes too thin or too short, it may not hold an implant firmly in place.
You need bone grafting when your jawbone does not have enough height or width to support a stable dental implant. Your dentist checks your bone with exams and 3D scans to see if it can anchor the implant safely.
If the bone looks strong and thick enough, you may not need a graft at all.
Bone grafting rebuilds weak areas so your implant can last. It creates a solid base that helps the implant stay secure when you chew and speak. Knowing when a graft is truly needed helps you avoid delays, extra costs, and future problems.
Key Takeaways
- Dental implants need enough healthy bone to stay stable.
- Bone grafting rebuilds areas where bone is too thin or too short.
- A detailed exam and imaging decide if you need a graft.
Understanding Bone Loss and Implant Stability
Bone loss changes the shape and strength of your jaw. If your jawbone is too thin or soft, your dental implant may not stay stable or heal the right way.
How Bone Loss Affects Dental Implant Success
Dental implants depend on osseointegration. This means the implant must fuse directly with your jawbone.
If you have bone loss, the implant may not have enough bone to grip. Without strong support, the implant can loosen or fail to heal fully. Early movement during healing raises the risk of implant failure.
Dentists look at three key factors before placing implants:
- Bone height
- Bone width
- Bone density
If any of these are too low, implant success drops. Research on factors affecting bone loss in dental implants shows that too much bone loss around an implant can lead to failure over time.
When your bone volume is low, your dentist may suggest bone grafting. A graft rebuilds lost bone and gives the implant a stronger base.
Causes of Jawbone Deterioration
Your jawbone needs regular pressure from chewing to stay strong. When you lose a tooth, that pressure stops.
The body then begins to break down unused bone. This process can start within months after tooth loss.
Common causes of bone loss include:
| Cause | How It Leads to Bone Loss |
| Missing teeth | No chewing pressure on the bone |
| Trauma or injury | Direct damage to bone tissue |
| Ill-fitting dentures | Uneven pressure and irritation |
| Long-term infection | Gradual destruction of bone |
You can still get implants in many cases. Options like grafting and advanced techniques make dental implants with bone loss possible for many patients.
Early treatment helps limit further damage.
The Role of Gum and Periodontal Disease
Gum disease is one of the main causes of bone loss in adults. When plaque builds up, it can turn into infection.
If the infection spreads below the gum line, it becomes periodontal disease. This condition attacks the tissue and bone that hold your teeth in place.
Over time, the bone shrinks and weakens. You may not notice pain at first, but signs can include:
- Bleeding gums
- Loose teeth
- Gum recession
If you plan to get dental implants, your dentist must control gum disease first. Active infection can stop proper osseointegration and reduce implant success.
Treating periodontal disease protects the remaining bone and improves your chances of long-term stability.
Book a consultation today to learn if your jawbone meets dental implant bone grafting requirements.
When Bone Grafting Is Needed for Dental Implants
You need enough healthy jawbone to hold an implant firmly in place. If your bone is too thin, soft, or short, bone grafting may be the only way to make implant placement safe and stable.
Signs You May Need Bone Grafting
You may need bone grafting if you lost a tooth months or years ago. After a tooth is removed, the jawbone in that area begins to shrink. The longer the space stays empty, the more bone you lose.
Gum disease is another common cause. Advanced periodontal disease can destroy the bone that once supported your teeth. Injury or trauma to the face can also reduce bone volume.
You might notice changes such as:
- A sunken look around missing teeth
- Dentures that feel loose
- Difficulty chewing on one side
In many cases, you will not feel bone loss at all. Your dentist often discovers it during an exam for implant dentistry. A bone graft rebuilds lost bone so your implant has a solid base.
How Dentists Assess Bone for Implant Placement
Your dentist does more than look at your gums. They measure bone height, width, and density before implant placement.
Most offices use digital X-rays and 3D imaging. A cone beam CT scan creates a detailed image of your jaw. This scan shows:
- Bone thickness
- Bone quality
- Location of nerves and sinuses
With 3D imaging, your dentist can see if the implant will have enough support. If the bone is too narrow or too soft, placing an implant without grafting increases risk.
Grafting adds volume and density to areas where bone has weakened. Your dentist uses this information to decide if you need grafting before moving forward.
This step protects you from preventable problems later.
Risks of Skipping Bone Grafting
You might feel tempted to skip bone grafting to save time or money. That choice can lead to implant failure.
An implant works like an artificial root. It must bond to your bone through a process called osseointegration. If the bone is too weak, the implant may loosen or fail to fuse.
Skipping grafting can lead to:
- Loose implants
- Ongoing pain
- Infection
- Need for implant removal
Implants placed in weak bone also face higher long-term stress from chewing. This stress can shorten the life of your restoration.
Research shows that many patients require grafting to avoid these problems. Building up the bone first gives your implant a stable foundation and lowers your risk of failure.
Contact our dental team to see whether bone grafting is needed before your dental implant procedure.
Types of Bone Grafting Procedures
Dentists use different bone graft methods based on how much bone you have lost and where the implant will go. The goal stays the same: rebuild enough strong bone to hold your implant in place.
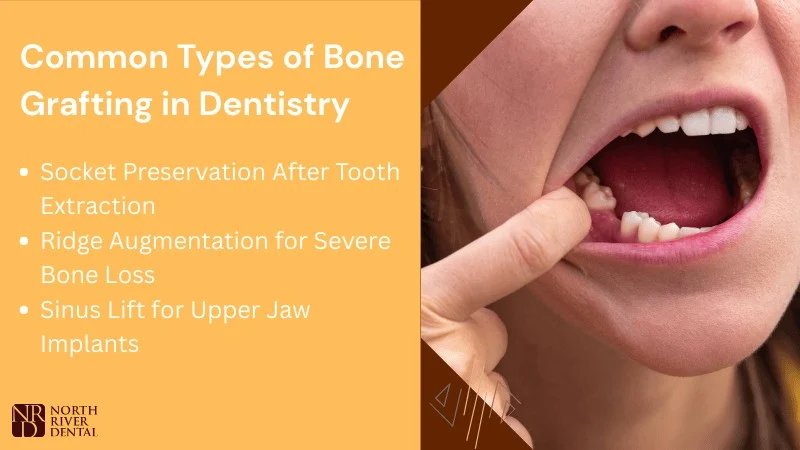
Socket Preservation After Tooth Extraction
When you remove a tooth, the bone around it starts to shrink within months. Socket preservation helps stop that early bone loss.
Right after the extraction, your dentist places a bone graft into the empty socket. The graft can come from your own bone, a donor, an animal source, or a synthetic material. It acts as a scaffold and supports new bone growth.
You may also receive a small membrane over the graft. This barrier keeps soft tissue from growing into the space meant for bone.
Healing usually takes a few months. If you plan ahead and choose socket preservation, you often avoid larger grafting procedures later.
Ridge Augmentation for Severe Bone Loss
If you lost a tooth years ago, your jaw may have become too narrow or too short for an implant. In that case, you may need ridge augmentation.
This procedure rebuilds the shape and width of your jawbone. Your dentist places a bone graft along the thin ridge to increase its size. Sometimes they use a block of bone. Other times they use small particles combined with a membrane.
Adding bone improves stability and helps the implant integrate with your jaw.
Healing can take four to six months or longer, depending on how much bone you need. You may need screws to hold the graft in place.
Ridge augmentation is more involved than socket preservation. But it often makes implants possible when bone loss is moderate to severe.
Sinus Lift for Upper Jaw Implants
If you need implants in your upper back teeth, you may face a different issue. The maxillary sinus sits just above that area.
After tooth loss, the sinus can expand downward. This leaves very little bone between your mouth and sinus cavity.
A sinus lift raises the sinus membrane and places a bone graft beneath it. This increases the height of bone so your implant has enough support.
Healing often takes several months. In some cases, your dentist can place the implant at the same time. In others, you wait until the graft fully integrates.
Sinus lifts are common and predictable when done by an experienced provider. They allow you to replace upper molars even when bone height is limited.
Bone Graft Materials and Techniques
Dentists choose graft materials based on how much bone you lost, where the implant will go, and your health history. Each option rebuilds jaw volume in a different way and heals at a different pace.
Autograft: Using Your Own Bone
An autograft uses bone taken from your own body. Your surgeon may take it from the back of your jaw, chin, or in rare cases, the hip.
Because the bone comes from you, your body accepts it well. It contains living cells and natural growth factors that help new bone form.
You get strong support for implants, especially if you have major bone loss. Many specialists view it as a reliable option for rebuilding jaw shape and density.
However, this method requires a second surgical site. That means more healing time and possible swelling in two areas.
Dentists often use autografts in larger defects, ridge augmentation, or when they need solid bone blocks instead of loose particles.
Allograft and Xenograft Options
An allograft uses donor bone from another person. Tissue banks clean and process it to ensure safety.
This option avoids a second surgery site. You heal in one area instead of two, which many patients prefer.
An allograft acts as a framework. Your own bone grows into it over time and replaces it.
A xenograft comes from animal bone, often bovine. It also goes through strict processing before use.
Dentists often use allografts and xenografts for socket preservation after tooth removal and for moderate bone loss.
Synthetic and Advanced Materials
Synthetic grafts use lab‑made materials such as calcium phosphate or hydroxyapatite. These materials mimic the mineral part of natural bone.
They provide structure and slowly dissolve as your body builds new bone. Because they are not taken from a person or animal, some patients feel more comfortable choosing them.
Your dentist may also use membranes during guided bone regeneration. These barriers protect the graft and keep soft tissue from growing into the space meant for bone.
A review of bone grafting techniques and materials for implant dentistry explains how different materials support implant stability.
Synthetic options work well for small to moderate defects. Healing time depends on the size of the graft and your overall health.
Working With Your Implant Specialist
Choosing the right implant specialist shapes your results. You need careful diagnosis, a clear treatment plan, and long-term support to protect your bone and preserve facial structure.

Why Periodontists Are Essential
You want a specialist who understands both gum health and bone biology. Periodontists focus on the tissues that support your teeth, including the jawbone that holds dental implants in place.
They receive advanced training in implant dentistry and bone grafting. This training helps them manage bone loss from gum disease, missing teeth, or injury.
A periodontist will:
- Measure your bone height and width
- Check gum health and infection risk
- Review medical conditions that affect healing
- Decide if grafting improves implant success
If you have moderate to severe bone loss, a periodontist often leads your care. Their goal is simple: create a stable base so your implant can fuse with bone and stay secure for years.
Personalized Treatment Planning
You should never get a one-size-fits-all plan. Your bone level, health history, and smile goals all matter.
Your specialist uses detailed exams and often 3D imaging to map your jaw. This helps them see thin areas of bone and plan the exact implant position.
Your plan may include:
- Immediate implant placement after extraction
- Bone grafting before or during implant surgery
- Use of short or narrow implants in select cases
- A staged approach with healing time between steps
If bone grafting is needed, your specialist will explain the type of graft and healing time. Most grafts need several months to build enough strength for implant placement.
Clear planning improves implant success and reduces the risk of loose implants or poor alignment.
Ensuring Long-Term Success and Facial Structure
Dental implants do more than replace teeth. They help preserve facial structure by supporting the jawbone.
When you lose a tooth, the bone in that area shrinks over time. This bone loss can change your facial shape and make you look older.
Your implant specialist works to:
- Maintain healthy bone around the implant
- Monitor gum health at follow-up visits
- Adjust your bite to avoid excess pressure
- Treat early signs of inflammation
Regular checkups protect your investment. With proper care, your implant can stay stable and support your facial structure for many years.
Frequently Asked Questions
You want clear answers before you move forward with a bone graft or dental implant. These common questions cover healing signs, timing, risks, and costs so you can make informed choices.
What are the signs of a successful dental bone graft procedure?
You should notice mild swelling and soreness for a few days, not severe pain. The area should slowly feel more normal each week.
Healthy gum tissue will look pink and closed over the graft site. You should not see exposed material or have ongoing drainage.
Your dentist may use 3D imaging to confirm the graft has bonded with your natural bone. CBCT scans often measure bone height and width before implant placement.
How can I expedite the healing process after a bone graft?
Follow your dentist’s instructions closely. Take prescribed antibiotics if given, and avoid smoking, which can slow bone healing.
Stick to soft foods for several days. Do not chew on the grafted side until your provider says it is safe.
Keep the area clean but do not brush directly over stitches unless told to do so. Rest, eat balanced meals, and manage health conditions like diabetes to support steady healing.
How long after a tooth extraction should I consider getting a bone graft?
Bone loss can begin soon after a tooth is removed. In many cases, dentists place a graft at the same visit as the extraction to limit shrinkage.
If you already had a tooth removed, schedule an exam as soon as possible. A provider can check bone volume and decide if you still have enough support for an implant without grafting.
Is there a time limit on how long a bone graft can stay viable without an implant?
A healed graft can remain stable for some time, but bone can slowly change if it does not support an implant. Your dentist will usually recommend placing the implant once the graft fully integrates, often within a few months.
Small grafts may heal in about three months. Larger grafts can take four to six months or longer before they are ready for an implant.
Delaying implant placement for too long may require a new evaluation to confirm the bone still has enough height and width.
What are the potential consequences of skipping a bone graft before dental implants?
If you do not have enough bone, the implant may lack stability. That can increase the risk of implant failure.
Insufficient bone can also affect the position of the implant. Poor placement may lead to bite problems or cosmetic concerns.
Modern techniques may allow treatment even with bone loss, but you still need enough support for long-term success.
How does the cost of dental bone grafting vary, particularly if multiple implants are involved?
Costs depend on the size of the graft, the material used, and whether you need sedation. A small graft for one site costs less than a large graft that rebuilds part of the jaw.
If you need multiple implants, you may also need a larger graft or procedures like a sinus lift. That increases total treatment costs.
Insurance coverage varies. Some dental plans limit graft benefits, and medical insurance may only help in specific cases, such as trauma-related bone loss. Always ask for a written treatment plan so you understand each fee before you begin.