Dental implants have a high success rate, but they can still fail. When an implant fails, you may notice pain, swelling, or movement where the tooth should feel solid.
In most cases, problems like infection, bone loss, smoking, health conditions, or poor placement cause the failure.
Dental implant failure usually happens because of infection, weak bone support, too much pressure on the implant, or health and lifestyle factors that slow healing.
You can lower your risk by choosing an experienced dental provider, keeping your gums clean, and following all post-surgery care instructions.
When you understand the dental implant failure causes, you take control of your results. Knowing the warning signs and how to prevent problems helps you protect your smile for years to come.
Key Takeaways
- Implant failure often links to infection, bone loss, excess pressure, or health risks.
- Early signs such as pain, swelling, or movement need prompt attention.
- Good oral hygiene and regular dental visits help protect your implant long-term.
Understanding Dental Implant Failure
Dental implants have a high success rate, but problems can still happen. You need to know what failure means, when it can occur, and how often it happens so you can act fast if something feels wrong.
Definition of Dental Implant Failure
Dental implant failure happens when the implant does not bond properly with your jawbone or stops working after it once felt stable. A failed dental implant may become loose, painful, or infected.
In many cases, failure means the implant did not fully fuse with the bone. This process is called osseointegration. If that bond does not form, the implant can move and cannot support a crown.
You may notice signs like swelling, bleeding, pus, or discomfort when chewing. Some people also see bone loss on an X-ray. When your dentist finds mobility in the implant, they usually remove it to prevent more bone loss.
Early vs. Late Dental Implant Failure
Dentists group dental implant failure into two types: early implant failure and late implant failure.
Early implant failure often happens within the first few months after placement. It usually occurs before the final crown goes on. Causes may include:
- Infection at the surgical site
- Poor bone quality
- Too much movement during healing
- Uncontrolled health issues like diabetes
A review of the etiology of dental implant failure explains that infection and instability play major roles in early failures.
Late implant failure can occur 1 to 3 years after implantation or even after many years. It often links to:
- Peri-implantitis (gum infection around the implant)
- Excess pressure from teeth grinding
- Poor oral hygiene
- Loose or poorly fitted restorations
Late failure often starts slowly, with bone loss around the implant.
Prevalence and Success Rates
Dental implants remain one of the most reliable tooth replacement options. Most studies show high long-term success rates.
Even so, failure is possible. Some reports note that problems can increase over time, especially if you smoke, skip dental visits, or have gum disease.
You lower your risk when you:
- Keep your gums clean
- Control medical conditions
- Attend regular dental checkups
- Follow post-surgery care instructions
When you understand how and why dental implants fail, you can spot problems early and protect your investment in your smile.
Contact our Ellenton, FL dental team today to discuss symptoms such as pain or looseness and get expert guidance before the problem worsens.
Major Causes of Dental Implant Failure
Dental implants fail when the bone does not bond to the implant, when gum disease damages the tissue around it, or when health problems slow healing.
Knowing these causes of dental implant failure helps you act early and protect your investment.

Poor Osseointegration
Osseointegration means your jawbone grows tightly around the implant and locks it in place. When this bond does not form, the implant can loosen or shift.
This problem is called poor osseointegration, and it is one of the main causes of implant failure.
Early implant failure often happens before your final crown goes on. You may notice movement, pain, or swelling.
In many cases, the body does not accept the implant due to low bone quality, surgical trauma, or infection during healing, as explained in this overview of dental implant failure causes.
Smoking, lack of bone volume, and excess pressure on the implant can also stop proper bonding. If the implant does not stay still during healing, the bone cannot attach firmly.
Peri-Implantitis and Gum Diseases
Peri-implantitis is a gum infection that damages the soft tissue and bone around your implant. It often starts as mild gum inflammation and can progress to bone loss if you do not treat it.
This condition is similar to periodontitis around natural teeth. Bacteria collect along the gum line, especially if you skip brushing and flossing. You might notice bleeding gums, bad taste, pus, or slight implant movement.
If bone loss continues, the implant can fail.
For the pre-implantitis treatment, regular cleanings and careful home care lower your risk. If you have a history of periodontitis, you face a higher chance of gum infection around implants.
Infection and Systemic Health Conditions
Infection is one of the most common causes of dental implant failure. Bacteria can enter the site during surgery or while the implant heals.
Health issues also play a role. Certain systemic health conditions reduce your body’s ability to heal and fight infection. These include:
- Uncontrolled diabetes
- Osteoporosis
- Immune disorders
- Long-term steroid use
Research shows that both local infection and underlying medical problems increase the risk of implant problems, including early and late failure.
If your blood sugar is not stable, healing slows and infection risk rises. When you manage your health conditions and follow your dentist’s instructions, you improve your chances of long-term implant success.
Surgical and Mechanical Factors
Surgical errors and bite forces can weaken the bond between your implant and bone. When stability drops, you may notice implant mobility, soreness, or even a loose implant.
Poor Surgical Technique
Your implant must lock into bone at the time of placement. Dentists call this primary stability, and it plays a key role in long‑term success.
If the surgeon overheats the bone, uses poor drilling technique, or places the implant at the wrong angle, the bone may not heal well around it.
Research shows that surgical trauma and bone quality strongly affect early failure, as explained in this review on causes and treatment of dental implant failure.
You may also face problems like dehiscence, where bone does not fully cover the implant. This leaves threads exposed and raises the risk of infection and implant looseness.
Careful planning with scans, proper irrigation during drilling, and correct implant positioning in the maxilla or mandible reduce these risks.
Insufficient Bone Density or Volume
Your implant needs enough bone density and bone volume to stay stable. If the jawbone is thin or soft, the implant may not anchor firmly.
Low density bone is common in the upper jaw, or maxilla. The lower jaw, or mandible, usually has denser bone, but bone loss can still occur after missing teeth for a long time.
When bone volume is limited, your dentist may suggest:
- Bone grafting
- Ridge augmentation
- Sinus lift procedures (in the upper jaw)
These steps rebuild support before implant placement. Studies show that poor bone quality and limited volume raise the risk of early failure, as outlined in this review of implant failure causes and management.
Without enough support, you may notice implant mobility during healing. A loose implant often needs to be removed before a new one can be placed.
Occlusal Overload and Bruxism
Your implant must handle normal bite forces. When forces exceed the bone’s tolerance, problems develop.
Occlusal overload happens when biting pressure is too strong or uneven. This can occur from poor crown design, missing back teeth, or bite misalignment.
If you grind your teeth at night, called bruxism, you place repeated stress on the implant. Over time, this stress can cause bone loss around the implant and lead to implant looseness.
Reviews on implant failure note that occlusal overload and bruxism are linked to late implant failure, including findings summarized in this scoping review of dental implant failure.
You can lower this risk by wearing a night guard, adjusting your bite, and placing enough implants to spread out force. Careful prosthetic design helps protect long‑term implant stability.
Book your dental implant consultation in Ellenton, FL to identify risk factors early and protect your investment from implant failure.
Warning Signs and Complications
Dental implants usually heal with mild soreness and swelling that improves each day. When symptoms get worse instead of better, your body may be signaling a problem that needs attention.
Signs of Dental Implant Failure
You should expect light swelling and mild pain for a few days after surgery. That discomfort should slowly fade. If pain grows stronger, lasts for weeks, or returns after healing, take it seriously.
Common signs of dental implant failure include:
- Ongoing swelling or redness around the implant
- Bleeding when you brush near the site
- Pus, discharge, or a bad taste in your mouth
- A feeling that the implant is not stable
A healthy implant feels firm. During healing, the bone should fuse to the implant. If that bond fails, the implant may not anchor properly. Do not ignore small changes. Early treatment often prevents bigger problems.
Gum Recession and Implant Mobility
Your gums should sit snugly around the implant and abutment. When gum recession develops, the metal post or abutment may become visible.
Receding gums can expose rough surfaces where bacteria collect. This raises the risk of infection around the implant. You may also notice tenderness when brushing.
A loose dental implant is more serious than a loose crown. Sometimes only the abutment or crown screw loosens, which your dentist can tighten.
But if the implant post itself moves, the bone may not have fused correctly.
If you feel movement, call your dentist right away. Waiting can lead to bone loss.
Difficulty Chewing and Pain

You should be able to chew without sharp or lingering pain once healing ends. Mild pressure may feel different at first, but it should not hurt.
Difficulty chewing on the implant side may signal a problem with how your bite fits together. Too much force on the implant can strain the bone and surrounding tissue.
Watch for:
- Pain when biting down
- Sensitivity that does not improve
- A dull ache that spreads to nearby teeth
Pain is your body’s warning system. If chewing feels wrong or uncomfortable, schedule an exam before the issue grows worse.
Prevention and Long-Term Care
You can lower your risk of implant problems with careful planning, daily cleaning, and steady follow-up care. The steps you take before and after surgery play a direct role in how well your implant heals and lasts.
Pre-Surgical Planning and Assessment
Strong planning helps prevent dental implant failure before surgery even begins. Your implant dentist should review your full health history, current medications, and habits like smoking or teeth grinding.
You may need X-rays or 3D scans to check bone height and width. Low bone volume, untreated gum disease, or uncontrolled diabetes can raise your risk of early failure.
Your dentist should also review all tooth replacement options, including partial dentures or bridges, so you can make an informed choice. Not every patient is a good candidate for implants right away.
Clear treatment planning matters for long-term success. Proper implant position supports stable implant restorations and lowers the risk of overload, screw loosening, and bone loss later on.
Speak directly with our Ellenton, FL implant team to review your symptoms, understand possible causes, and take the next step toward saving your implant.
Oral Hygiene and Maintenance
Poor oral hygiene is a leading cause of peri-implant disease. Bacteria can build up around the implant and lead to inflammation and bone loss.
Research in the review on dental implant failure and peri-implantitis explains how plaque buildup around implants can trigger infection and tissue damage.
You should brush twice a day with a soft brush and clean between teeth with floss or interdental brushes. Pay close attention to the gum line around the implant restoration.
Professional cleanings are not optional. Visit your implant dentist at least once a year, or more often if you have a history of gum disease.
Watch for warning signs:
- Bleeding when brushing
- Swelling around the implant
- Bad taste or odor
- Slight movement of the implant
Report these signs early to protect your implant restorations.
Managing Risk Factors and Aftercare
Certain habits increase your risk of late implant failure. Smoking, uncontrolled diabetes, and bruxism can weaken bone support over time.
If you grind your teeth at night, ask your dentist about a night guard. It reduces excess force on the implant and lowers the risk of fractures or screw loosening.
Follow all post-surgical care instructions closely. This often includes:
- Taking prescribed medications as directed
- Avoiding hard foods during early healing
- Keeping the surgical area clean but not disturbed
Skip heavy chewing on the implant side until your dentist confirms full healing. Strong aftercare and regular exams protect your implant restoration and help you avoid preventable complications.
Treatment and Solutions for Failed Implants
When a dental implant fails, you still have clear treatment paths.
Your dentist will first remove the failed implant and control infection, then decide if re-implantation or another tooth replacement option fits your needs.
Implant Removal and Re-Implantation
If your implant feels loose, causes pain, or shows bone loss on an X-ray, your dentist will plan implant removal. Signs like swelling, bleeding, or pus often point to infection.
You can read more about common warning signs in this guide on dental implant failure signs and causes.
Your dentist removes the implant to stop further bone loss. Quick action protects the jaw and makes future treatment easier.
After removal, you may need:
- Bone grafting to rebuild lost bone
- A healing period of several months
- Careful control of gum infection
Once the area heals, you can move forward with re-implantation. Your dentist may use a wider implant or improve placement to increase stability.
Better oral hygiene, smoking control, and managing health conditions like diabetes can lower the risk of another failure.
Alternative Tooth Replacement Options
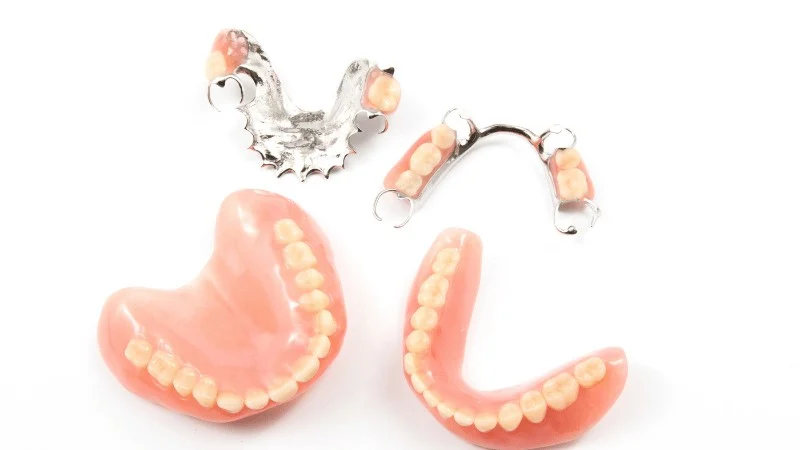
If re-implantation is not a good choice, you still have reliable tooth replacement options.
Common options include:
- Dental bridges, which attach to nearby teeth
- Removable partial dentures
- Full dentures if several teeth are missing
Bridges work well if the teeth next to the gap are strong and healthy. Dentures cost less than implants and avoid surgery, but they may feel less stable.
Your dentist will review your bone level, gum health, budget, and long-term goals.
If you have ongoing gum disease or repeated implant problems, choosing a non-implant option may protect your oral health and reduce future complications.
Frequently Asked Questions
Dental implant failure can happen because of infection, bone loss, excess pressure, or health issues like smoking and diabetes.
You can lower your risk when you know the warning signs and understand how location and habits affect healing.
What are the common reasons for dental implant failure?
The most common cause is infection around the implant. Bacteria can build up and lead to bone loss, a condition called peri‑implantitis, as explained in this review on the etiology and management of dental implant failure.
Poor bone quality or weak bonding between the implant and your jaw can also cause early failure. Surgical problems, too much pressure from biting, and uncontrolled health conditions increase the risk.
How can you recognize early signs of implant failure?
You may notice pain that does not improve after healing time. Swelling, bleeding, or pus around the implant are also warning signs.
An implant that feels loose is a serious red flag. Healthy implants should not move at all.
Bad taste, gum redness, or gradual bone loss seen on X‑rays can point to early peri‑implant disease. Call your dentist right away if you notice these changes.
Is dental implant failure possible years after the procedure?
Yes, late failure can happen even after years of normal use. It often links to long‑term infection, bone loss, or repeated heavy biting forces.
Studies show that problems like screw loosening or bone loss can increase over time. Teeth grinding, also called bruxism, adds extra stress to the implant.
Regular checkups help catch small problems before they lead to implant loss.
Can you get a refund if your dental implant fails?
Refund policies depend on your dentist and the written agreement you signed. Some offices offer limited warranties for a set number of years.
Many clinics will assess the cause before offering repair, replacement, or partial credit. Failure caused by smoking, poor oral care, or missed visits may not qualify.
Review your treatment contract and talk directly with the office manager for clear details.
How does smoking affect the success rate of dental implants?
Smoking slows healing and reduces blood flow to your gums. This makes it harder for the implant to bond with your bone.
It also raises your risk of infection and bone loss. Research consistently lists smoking as a major risk factor for implant failure.
If you quit before and after surgery, you improve your chances of long‑term success.
Which location in the mouth has the highest risk of implant failure?
Implants in the upper jaw often carry a higher risk. The bone in the back upper jaw is usually softer and less dense.
Low bone density can make it harder for the implant to stay stable during healing. Sinus space in the upper back area can also limit available bone.
Your dentist may suggest bone grafting or a sinus lift if this area lacks enough support.